A bedsore lawyer at Wieand Law Firm will fight for the rights of elderly nursing home victims who suffer painful ulcers due to neglect. If you or a loved on has suffered a bedsore as the result of substandard medical care at a nursing home, a Philadelphia bedsore lawyer can help you receive fair compensation for harms and losses suffered.
Bedsores are injuries to skin and underlying tissue that are caused by prolonged pressure on the skin that limits blood flow. Bedsores are also known as pressure sores or pressure ulcers. Frequently, bedsores develop on skin that covers bony areas of the body, such as the heels, ankles, hips, and tailbone. In nursing homes, residents who are confined to a wheelchair or bed are at the highest risk of bedsores due to their inability to change positions.
A Philadelphia bedsore lawyer can advocate for elderly nursing home residents who have been neglected or abused. To schedule a free consultation with a nursing home lawyer call us at (215) 666-7777.
Pressure sores often result from pressure combined with pulling on the skin, friction, and moisture, particularly over bony areas. For example, bedsores may form on the buttocks of wheelchair-bound residents that spend an extended amount of time in the same position. Bed sores also frequently form on boney areas such as the heal.
You should consult with a Philadelphia bedsore lawyer if your loved one is suffering from a pressure ulcer. They may be entitled to compensation for their pain and suffering.
Bedsores are often preventable if proper care is taken by nursing home staff. Nursing homes must take meticulous care of residents that are at high risk for developing bedsores. The way for nursing staff to prevent pressure sores is by keeping the skin clean, dry, and free of pressure. To prevent ulcers from forming, residents should be encouraged to move around the facility. Bed-bound or wheelchair-bound patients should be repositioned every few hours. A pressure-reducing mattress or bed may be needed for residents that have recurring or severe bedsores. Nursing homes should conduct regular physical examinations of residents at risk for pressure ulcers.
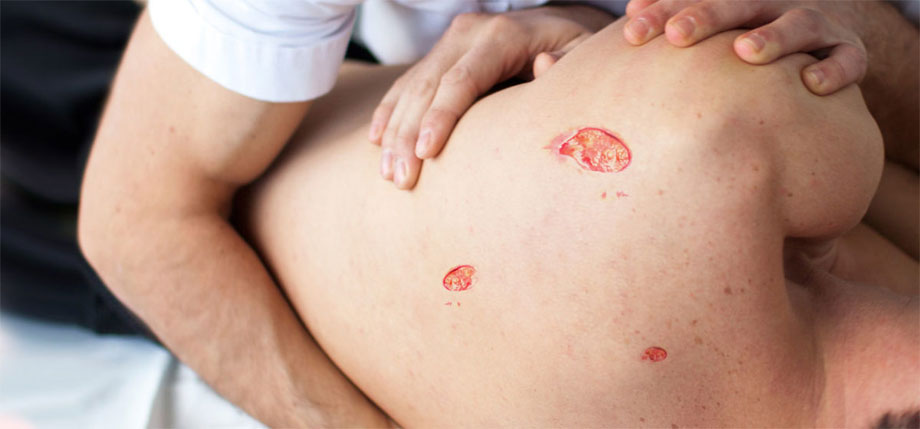 If a nursing home resident develops a pressure ulcer, nursing staff should quickly assess and intervene with treatment. After a bedsore has developed, treatment includes cleansing, removal of pressure from the affected area and application of special dressings. With prompt treatment, early-stage pressure sores will usually heal. However, if the bedsore does not heal after conservative treatment, sometimes surgery is needed.
If a nursing home resident develops a pressure ulcer, nursing staff should quickly assess and intervene with treatment. After a bedsore has developed, treatment includes cleansing, removal of pressure from the affected area and application of special dressings. With prompt treatment, early-stage pressure sores will usually heal. However, if the bedsore does not heal after conservative treatment, sometimes surgery is needed.
Different stages are used to describe the extent of damage to the skin and tissue caused by bedsores.
Some bed sores are graded “unstageable” because the stage cannot clearly be determined. This may happen when a thick layer of other tissue and pus covers the sore and the base of the sore cannot be viewed to determine the stage. In stages 3 and 4, serious complications such as osteomyelitis or sepsis can occur. For this reason, patients may be prescribed a topical or oral antibiotic to treat infected pressure sores that aren’t responding to other treatment. In addition, bedsores that reach advanced stages may require surgical amputation to cut away dead tissue which helps with the healing process.
Bedsores are frequently preventable. A Philadelphia bedsore lawyer can hold nursing homes that provide substandard care accountable.
The development and progression of bedsores in nursing home residents may indicate negligent care on the part of a nursing home. Federal and state laws require that nursing home provide care that ensures a resident’s well-being and safety. If a nursing home facility does not take all appropriate measures to prevent and treat bedsores, they can be held liable in court for resulting damages.
The Wieand Law Firm fights for justice for victims who are injured as a result of negligent nursing home care. If a loved one has developed bedsores call, speak with an experienced bedsore lawyer at the Wieand Law Firm to investigate a lawsuit against the facility.
– Results may vary depending on your particular facts and legal circumstances
Review: 5/5
★ ★ ★ ★ ★
“Attorney Brent Wieand is the ! I trust him to handle all my legal problems, big or small!”
-Sasha Bharrat
