 Pressure ulcers, informally called “bedsores,” are often linked as an indication of neglect for nursing home or personal care home residents. Pressure ulcers can develop when needed care, such as repositioning residents with mobility deficits, is not provided. If you believe that you or a loved one developed a pressure ulcer due to caregiver negligence, nursing home pressure ulcer lawyers at the Wieand Law Firm can pursue compensation for your losses.
Pressure ulcers, informally called “bedsores,” are often linked as an indication of neglect for nursing home or personal care home residents. Pressure ulcers can develop when needed care, such as repositioning residents with mobility deficits, is not provided. If you believe that you or a loved one developed a pressure ulcer due to caregiver negligence, nursing home pressure ulcer lawyers at the Wieand Law Firm can pursue compensation for your losses.
At the Wieand Law Firm, we represent victims of bedsore injuries and their families. Bedsores are both serious and devastating. Notoriously difficult to heal, pressure ulcers expose their victims to many complications such as infections, sepsis, and even death. Nursing home lawyers Philadelphia PA counts on will fight to get you or your loved one the proper care and maximum compensation for your injuries.
Our team of nursing home pressure ulcer lawyers understand the causal links between negligence and bedsores. When pressure ulcers occur due to negligence and failure to uphold care standards, the victim is entitled to compensation for their injuries. The nursing home lawyers Philadelphia PA trusts at the Wieand Law Firm will evaluate your case and injuries, calculate your damages, and determine which parties may be held accountable.
Pressure ulcers are defined as wounds on the skin and underlying tissue resulting from a sustained period of pressure. Pressure ulcers frequently occur on skin areas that cover bony prominences, such as the sacrum, ankles, heels, and spine. Pressure ulcers can be difficult to heal, increase resident’s infection risk, be a source of pain or discomfort, and sometimes lead to death.
There are four stages of pressure ulcers, which delineate the ulcer’s severity. Stage I pressure ulcers denote intact skin with signs of pressure. A sign of pressure for stage I ulcers include reddened skin that doesn’t turn white when touched. In the next stage, the skin (dermis) opens or develops a blister; this is called a Stage II ulcer. Stage III pressure ulcers are even more serious, denoting full thickness loss of both the skin and subcutaneous tissue below it. Finally, Stage IV ulcer is when a pressure ulcer becomes so deep that it expands into the muscles, tendons or bone.
Pressure ulcers can be extremely difficult to heal. That’s why it’s crucial that the health care professionals responsible for the care of at-risk residents take all recommended precautions to prevent pressure ulcers. Sadly, the nursing home pressure ulcer lawyers at our firm have witnessed many cases in which nursing homes fail to initiate or consistently implement pressure reduction measures, and residents sustain serious harm.

Conducting a complete risk assessment for skin breakdown is a critical first step in prevention. Many nursing homes use a standardized assessment called the Braden Scale to ascertain a patient’s risk of skin breakdown. If a resident is identified from the Braden Scale as an at-risk resident, urgent action must be taken to minimize the risk of breakdown. Personalized interventions may include pressure reducing support surfaces, such as a specialized mattresses or wheelchair cushions.
Turning and repositioning schedules must be implemented and tailored based on the resident needs. Facilities that cite a standard 2-hour repositioning schedule should be questioned on how this schedule is monitored and documented. All too often, nursing facilities fail to maintain consistency with this repositioning schedule. Additionally, some residents who have a high risk for skin breakdown might require repositioning more frequently in order prevent pressure injury.
Unfortunately, the nursing home pressure ulcer lawyers at the Wieand Law Firm see cases in which facilities fail to implement these important skin-saving measures due to cost, lack of staffing, or a knowledge deficit.
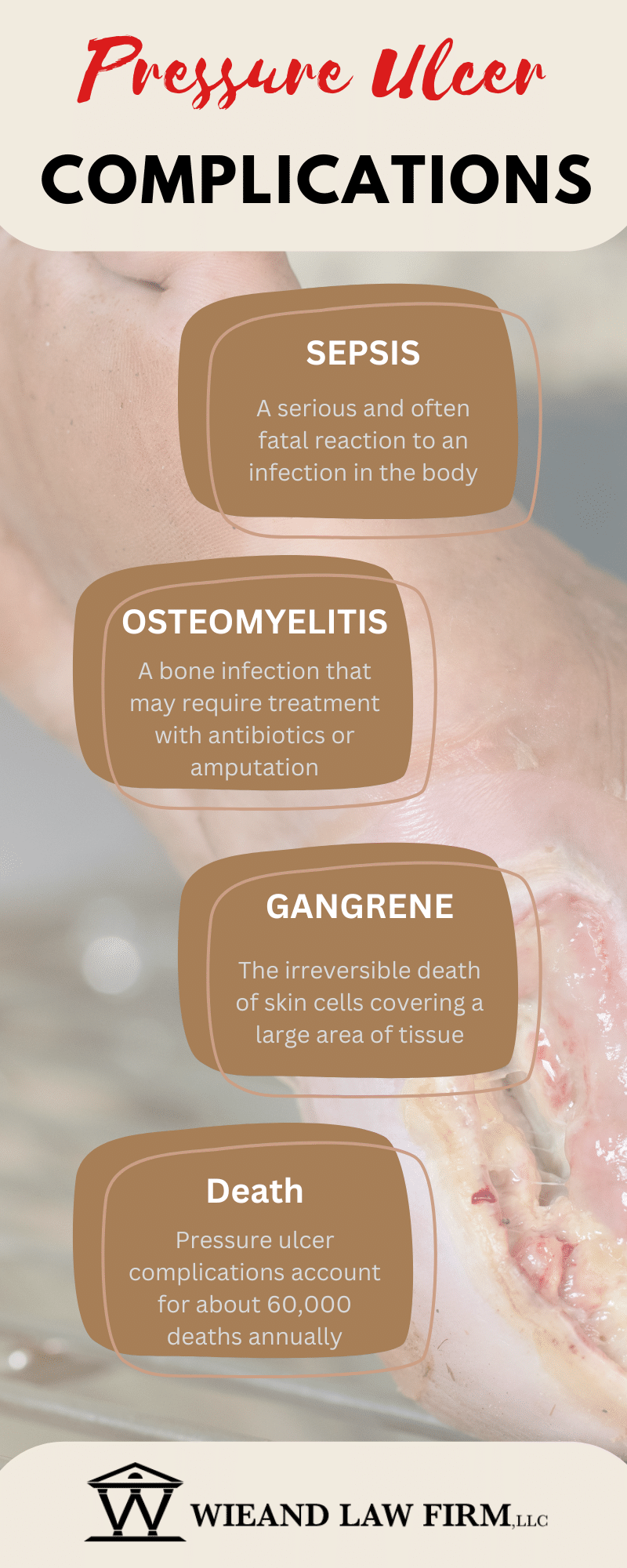 Pressure Ulcers Complications
Pressure Ulcers ComplicationsPressure ulcers are a huge risk to a resident’s health and can lead to serious complications. Wounds that become infected can prolong the length of time for wound healing and require the use of medications such as antibiotics. Untreated infections can result in a bone infection known as osteomyelitis, or lead to sepsis, a life-threatening multi-organ response to an infection. Additionally, pressure ulcers frequently cause significant pain and suffering for residents. Complications of bedsores include:
Complications from pressure ulcers can require aggressive, invasive, and paintful treatments. Some patients who develop severe infections may require an amputation of the affected area. Contact the bedsore lawyers at the Wieand Law Firm for help if you or a loved one suffered any of these complications from a preventable pressure ulcer injury.
A nursing home is liable for pressure ulcers when it fails to act within established standards for preventing and treating bedsores. Liability for pressure ulcers is unique to each case and the specific circumstances surrounding the injury. Sometimes, more than one party is responsible for the action, or inaction, that resulted in the development of the pressure ulcer.
Some of the parties that may be held liable for a pressure ulcer injury may include:
Contact the nursing home pressure ulcer lawyers at the Wieand Law Firm for a free case review and evaluation. Our seasoned bedsore lawyers can help identify the liable parties and file a complaint on your behalf.
There is often a causal link between pressure ulcers and understaffing in nursing homes. Understaffing is one of the biggest and most prevalent causes of nursing home neglect. Bedsores are often a visual indicator and result of nursing home neglect from understaffing.
Residents who live at understaffed nursing homes are at higher risk of developing pressure ulcers. While anyone can develop a pressure ulcer, residents with mobility problems and nutritional issues are at even greater risk. When nursing homes fail to provide necessary mobility assistance and nutritional supports, they can be held liable when a pressure injury occurs.
Like many other medical complications facing nursing home residents, pressure ulcers are frequently caused by inadequately trained staff. Nursing homes frequently fail to educate staff members about pressure ulcer prevention and treatment. Staff members may fail to identify pressure sores at early stages or may fail to initiate proper interventions as part of the plan of care.
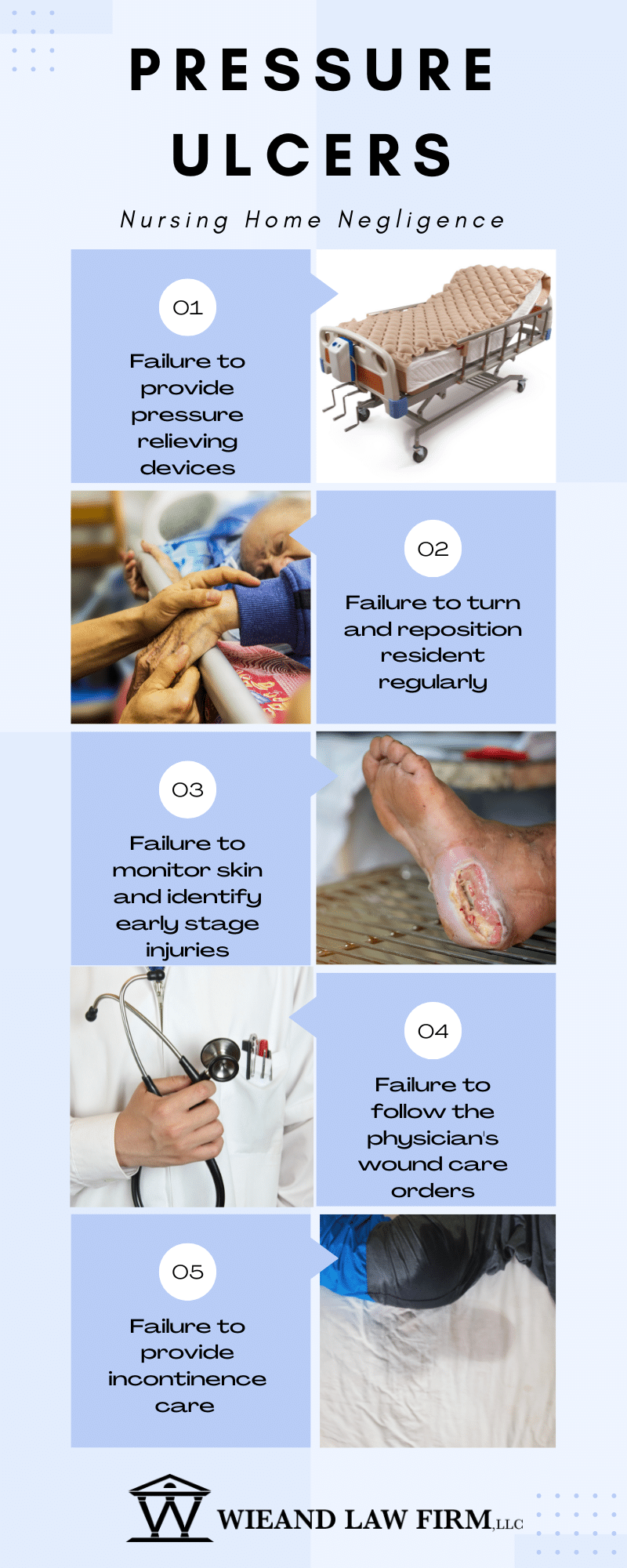
 Examples of Nursing Home Negligence for Bedsores
Examples of Nursing Home Negligence for BedsoresNursing home lawyers Philadelphia PA relies on have investigated and litigated many bedsore lawsuits. Examples of nursing home negligence that cause bedsores include:
Without proper care, bedsores can quickly progress and deteriorate to severe wounds. Bedsore lawyers at the Wieand Law firm holds nursing homes, assisted living facilities, and hospitals liable when their negligence results in serious patient injury.
 How Do Bedsore Lawyers Prove Liability?
How Do Bedsore Lawyers Prove Liability?To win a pressure ulcer lawsuit, you must be able to prove that the nursing home was legally responsible, or liable, for the injury. To accomplish that, you must establish four standard elements in the case:
The nursing home pressure ulcer lawyers at our firm have years of experience in these types of cases. Our attorneys understand the standards that nursing homes must follow and how to identify if a standard of care is breached.
Nursing home litigation is complex and challenging. The nursing home lawyers Philadelphia PA trusts at the Wieand Law Firm have exceptional insight into the state and federal regulations governing nursing homes. Our team partners with industry experts in wound care, nursing home management, and a variety of other specialties to investigate and support your claim.
Most pressure ulcers can be prevented with proper care. Bedsores are often a result of negligence. More than 17,000 lawsuits are filed each year related to pressure ulcers. In fact, lawsuits related to pressure ulcers are one of the most common personal injury lawsuits.
If you believe that your loved one suffered a pressure ulcer because a nursing home or assisted living failed to provide the proper standard of care, reach out to nursing home pressure ulcer lawyers for a free case review and evaluation.
Personal injury lawsuits in each state have a specific statute of limitations that restrict the time you have available to file a claim. Because nursing home cases are complex and can take time to thoroughly investigate, consider speaking with an attorney as soon as feasible to preserve your rights.
 What Damages Can You Recover from a Pressure Ulcer Lawsuit?
What Damages Can You Recover from a Pressure Ulcer Lawsuit?Medical care for pressure ulcers in the United States is expensive. According to the Agency for Healthcare Research and Quality, patient care costs per pressure ulcer can range from $20,900 to $151,700. A pressure ulcer lawsuit is a way to recover financial compensation for the damages sustained from nursing home negligence.
A study entitled Long-Term Care Liability for Pressure Ulcers published in the Journal of the American Geriatrics Society found residents and their families achieved recovery against the nursing facility in 87% of pressure ulcer lawsuit cases.
Pressure ulcer lawsuits settle for an average of $250,000 – $450,000. When the lawsuit proceeds to a trial, the average jury awards average closer to $1,000,000 or more.
Nursing home pressure ulcer lawyers at the Wieand Law Firm can seek different types of damages based on your individual case. These damages may include:
Contact nursing home lawyers Philadelphia PA relies on to discuss the specifics of your case and find out if you are eligible to file a lawsuit for damages.
Over 60,000 people per year die from pressure ulcer injuries and their complications. Many of these deaths occur when the pressure ulcer isn’t properly treated and develops a bacterial infection. Risk of death from bedsores significantly increased when the wound progresses to Stages III or IV.
If your loved one died from a bedsore caused by a negligent nursing home, you can file a wrongful death claim to hold the facility liable and seek recovery for their losses. Wrongful death claims can help you recover compensation for medical bills, pain and suffering, loss of consortium, and funeral and burial costs.
 Reasons to Hire the Wieand Law Firm
Reasons to Hire the Wieand Law FirmThe bedsore lawyers at the Wieand Law Firm aggressively fight for maximum compensation for resident’s whose health has been harmed by a pressure ulcer. Nursing homes have professional legal teams that have the sole goal to minimize awards of pressure ulcer sufferers. That’s why you need the support of a trusted nursing home attorney to seek fair compensation for injuries caused by preventable pressure ulcers. The Wieand Law Firm will take the time to listen to your situation and provide that skilled advice you need to act.
The nursing home lawyers Philadelphia PA counts on can provide the guidance you need during this difficult time. Experienced bedsore lawyers, our team of attorneys can:
The bedsore lawyers at the Wieand Law Firm use a contingency fee agreement for nursing home negligence cases. We recognize that everyone should be able to afford qualified, professional legal services regardless of ability to pay.
By working on contingency, our nursing home pressure ulcer lawyers only receive a fee if we win money for your claim. And, that fee is earned as a percentage of the amount that we win for your claim. This allows our clients to hire the professional counsel they need without worrying about hefty lawyer bills.
 Call Today for a Free Case Evaluation
Call Today for a Free Case EvaluationNursing home lawyers Philadelphia PA trusts at the Wieand Law Firm offer a free case review and evaluation. This helps you to understand your legal options and find out more about the process of filing a lawsuit. To speak with nursing home pressure ulcer lawyers at the Wieand Law Firm call us today at 215-666-7777 to receive a free, no obligation consultation.
Disclaimer: This article is for informational purposes only and is not legal advice.
